What is the First Treatment for Cervicogenic Headaches?
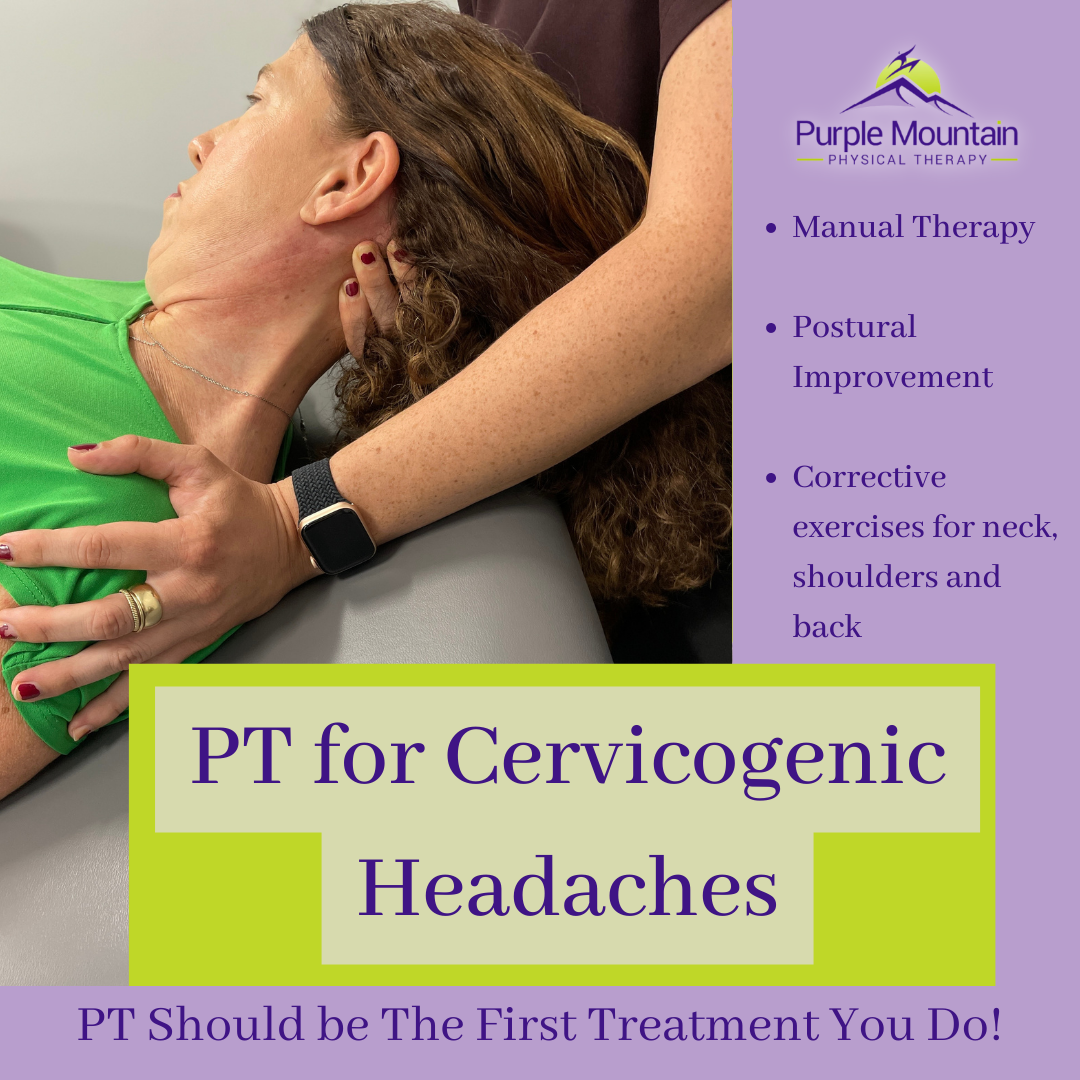
Did You Know that Physical Therapy is the First Treatment for Cervicogenic Headaches? One of the unique aspects about Purple Mountain Physical Therapy is that we have close connections to specialized physical therapists internationally who are devoted to providing excellent care to their patients, just as we are. When it comes to cervicogenic headaches, many […]