We treat women throughout their lifespan, helping them recover from their pelvic conditions, neck pain, TM joint disorders and headaches. We help you to get back to an active and vibrant life! We are expert pelvic health & orthopedic physical therapists, offering years of experience helping women just like you to recover. Our goal is to provide you compassionate, evidence-based care in a healing environment, that achieves your goals and gives you results. Some of the conditions we treat include:

- Pelvic Floor Dysfunction
- Stress Urinary Incontinence
- Urge Urinary Incontinence
- Urinary Frequency and Urgency
- Overactive Bladder
- Nocturia
- Sexual Health, Vaginismus, Dyspareunia
- Diastasis Rectus Abdominis (DRA)
- Osteopenia & Osteoporosis
- Menopause & Midlife Associated Pelvic Discomfort and Pain
- Perineal Pain and/or Anal pain
- Constipation
- Irritable Bowel Syndrome (IBS)
- Myofascial Pain Syndrome
- Interstitial Cystitis/Bladder Pain Syndrome
- Endometriosis Related Chronic Pelvic Pain
- Chronic Pelvic Pain
- Pelvic Organ Prolapse
- Cystocele, Rectocele, Uterine Prolapse, Rectal Prolapse.
- Sacroiliac Joint Pain (SIJ pain)
- Postpartum Recovery
- Pelvic Girdle Pain (both pregnancy and non-Pregnancy)
- Adductor, Groin and Hip Pain
- Hip Arthritis, Hip Labral Tears
- Vulvar Pain, Vulvodynia, Vestibulodynia
- Recurrent Urinary Tract Infection
- Lichen Sclerosus Related Pelvic Pain and Dysfunction
- Persistent Genital Arousal Disorder (PGAD)
- Clitorodynia
- Coccydynia (Coccyx Pain)
- Pudendal Neuralgia
- Dyspareunia (Painful Intercourse)
- Rehabilitation Following Hysterectomy
- Low back pain, SI joint disorders, neck pain and headaches
- Fecal Incontinence, Fecal Smearing, Flatulence Incontinence, Fecal Urgency
- High Tone Pelvic Floor
- Polycystic Ovarian Syndrome (PCOS) Associated Pain

Pelvic Floor Dysfunction: Pelvic floor dysfunction is a broad term that means the muscles of your pelvic floor are not working correctly. Your pelvic floor, also called your pelvic diaphragm, is a series of muscles that form a hammock at the base of your pelvis. They provide support to your organs and contribute to sexual function and urinary and fecal continence. When we evaluate your pelvic floor, we look for issues with the strength, tension, tone, length, contractile ability, functional lift capacity, speed and power of contractility and coordination of the pelvic floor with other key muscle groups. Pelvic floor dysfunction is at the heart of our specialty, as this is often present with all other pelvic problems, including chronic pelvic pain, stress urinary incontinence, urge urinary incontinence, overactive bladder, Pudendal neuralgia, dyspareunia (painful sex), endometriosis related chronic pain, incomplete bladder emptying and urinary urgency and frequency.
High tone pelvic floor: This is a type of pelvic floor dysfunction where the muscles have too much tone, which can also be thought of as too much stiffness. When this is the case a person will experience compromised function of the muscles because they cannot optimally contract, lengthen and return to a baseline, proper resting length. Sometimes there is confusion regarding high tone pelvic floor because it might be called other terms, such as pelvic floor spasm, overactive pelvic floor, pelvic floor hypertonicity, or pelvic floor contracture. High tone pelvic floor can lead to myriad symptoms including pelvic pain, urethral pain, dyspareunia (painful sex), vaginal pressure (feeling as if you have a pelvic organ prolapse), urinary urgency and frequency, stress urinary incontinence, urge urinary incontinence, overactive bladder, painful bladder syndrome/interstitial cystitis and other issues. Our treatment program for you will determine whether you have pelvic floor dysfunction or high tone pelvic floor. Next, if you do, we will work together to optimize your pelvic floor tone. Because the pelvic floor does not operate in isolation, you will receive a comprehensive evaluation of the muscles that coordinate with your pelvic floor, as well. We need to restore optimal function of all of these muscle groups to allow for the high tone pelvic floor to let go. With proper treatment for high tone pelvic floor you will notice you feel better and your pelvic symptoms (incontinence, pain, urgency, nocturia, etc.) will improve.
Bladder conditions and Urinary incontinence: This is a broad category of several problems causing the involuntary loss of urine. Yes, we treat:
Stress Urinary incontinence, Urge Urinary incontinence, Mixed incontinence
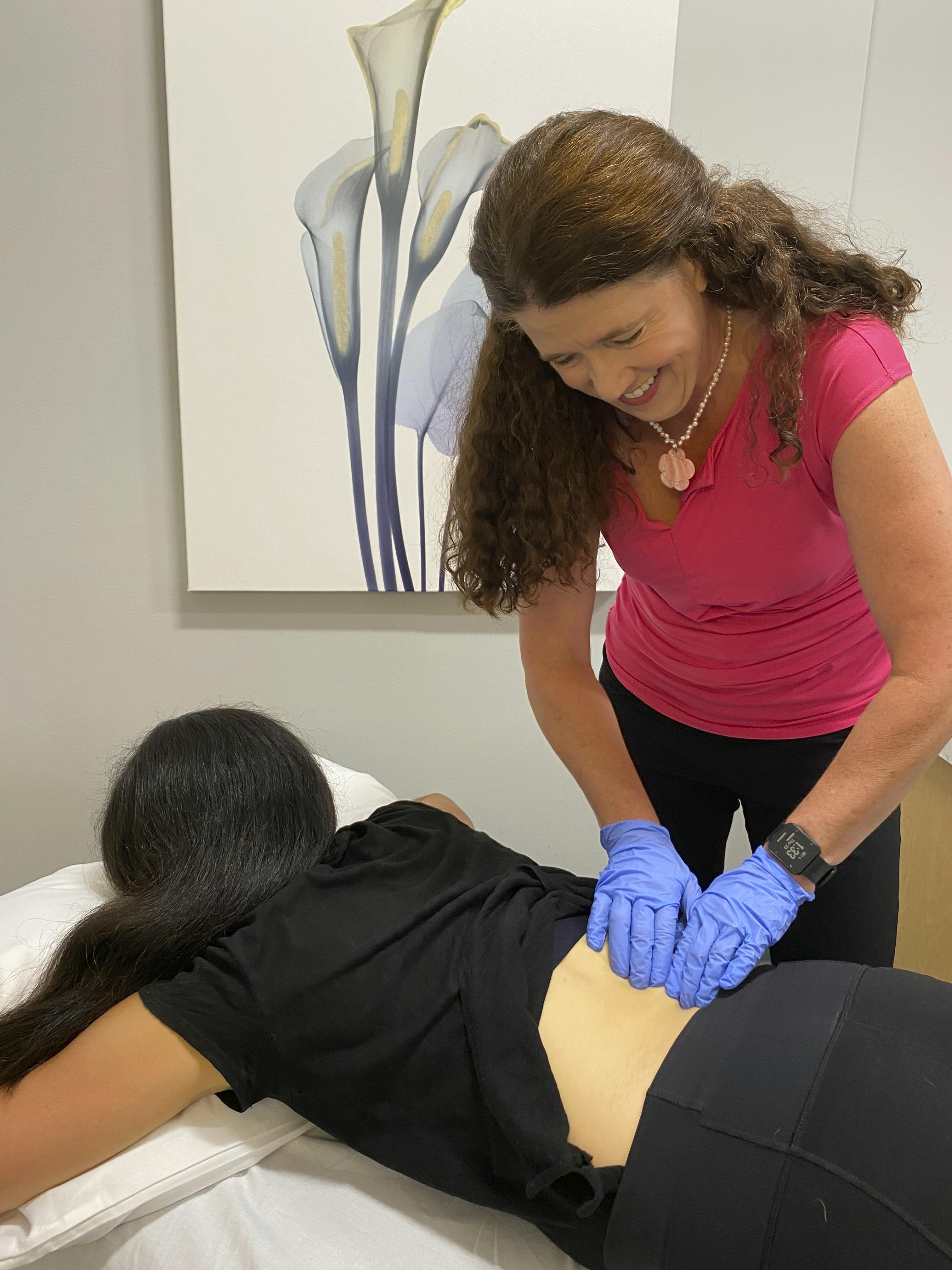
A thorough physical therapy evaluation, by the experienced pelvic health physical therapists at Purple Mountain Physical Therapy, will determine what’s going on and how to recover your control. Urinary incontinence is not exclusively a pelvic floor problem; therefore, Kegels alone cannot solve this. Your evaluation will be very helpful for you, many women report they’ve learned much about their bladder and their body and wish they had known this years ago so they could have avoided urinary incontinence. You will be provided with a customized treatment plan that delineates a realistic path forward for you to regain urinary control again. We will teach you exercises, educate you regarding optimal bladder habits and advise behavioral changes that contribute to your incontinence; these items have been proven through research to be one of the first things for you to do to help this problem!
Stress Urinary Incontinence: Stress urinary incontinence is the involuntary loss of urine that most of us have heard about and many women think is “normal” after you’ve had a baby or as you age. It is never normal to be leaking urine. Recovery of your urinary control is possible and with skilled physical therapy you will receive expert care and a customized treatment program to help you get back to walking, running, and exercise without incontinence. We will evaluate your breathing, abdominal wall, back muscles, hip girdles and pelvic floor and we will teach you how to coordinate muscular control to facilitate the return of continence. We will teach you how to properly engage your pelvic floor, addressing speed, power, pre-activation, coordination, release and all aspects of necessary pelvic floor function to optimize this muscle group’s ability to coordinate with the rest of your core muscles. We are experienced physical therapists with proven experience helping many people overcome their stress urinary incontinence.

Urge Urinary incontinence: Urge urinary incontinence occurs when your bladder muscle contracts strongly and your pelvic floor muscles cannot overcome this contraction, therefore urine unexpectedly comes out. The volume of urine lost during urge urinary incontinence varies from a few small drops to the entire contents of the bladder. We are here to help you recover your bladder control. Under the evaluation and treatment of the experienced pelvic health physical therapists at Purple Mountain Physical Therapy you will learn to overcome your urge incontinence and urinary urgency. We will evaluate not only your pelvic floor, but all areas related to bladder control, including your breathing, core muscles, low back, hip girdles and abdominal wall. We will teach you effective strategies to calm down your bladder and provide you with exercises that assist your recovery. We provide expert, hands-on treatment to treat the musculoskeletal contributions to your urge urinary incontinence.
Overactive Bladder (OAB) and Urinary urgency and frequency: Sometimes a bladder seems to have a mind of its own and a person must urinate much more often than normal. An overactive bladder has difficulty filling up with urine and storing the urine until the appropriate time to urinate. Physical therapy can help your overactive bladder and urinary urgency and frequency. There is a better way to live and there are proven, effective treatments to calm down this type of bladder! Yes, there is hope and this can get better! Wouldn’t it be nice to take a road trip and not have to stop at every opportunity? We are here to help you! We have heard from many of our patients that they have their life back following treatment. We’ve helped women wean off of their overactive bladder medications, as well. With the expert guidance of your pelvic health physical therapist at Purple Mountain Physical Therapy we will evaluate you and determine what is going on so we can develop a customized treatment approach for you.

Interstitial Cystitis/Bladder Pain Syndrome (BPS): Purple Mountain Physical Therapy is the right place to treat your interstitial cystitis and bladder pain syndrome! We’ve treated many people, men and women, who have IC/BPS. Yes, they improve. Yes, you can feel better. Yes, there is hope. We are experienced pelvic health physical therapists and we are here to help you. We have done the work: studying interstitial cystitis, pelvic pain and bladder conditions, attending professional conferences and even teaching other professionals advanced treatment techniques. We will evaluate you and, together, we will discover what is going on, what skilled treatment you require and how to make you feel better again. We will design you a custom treatment program for your interstitial cystitis/bladder pain syndrome, based in research backed treatments and rooted in over 20 years of experience working with individuals like you. We will teach you what you can do for yourself to feel better. In the skilled hands of your physical therapist you will find a path forward that actually works. Yes, even if you’ve had a cystoscopy that shows you have glomerulation or Hunner lesions, we can work with you and help you. Our treatment addresses your pain (whether it is pelvic pain or outside the pelvis) and bladder function so you feel better.
Pelvic Organ Prolapse (POP), Rectocele, Cystocele, Uterine prolapse, Rectal prolapse: Do you experience vaginal pressure, a feeling of heaviness, a sense that something is falling out of your vagina? With this pressure do you also experience back pain or sacroiliac joint (SIJ) pain, difficulty urinating or evacuating your stools? These are some of the symptoms of a pelvic organ prolapse. A prolapse is a condition when there is descent of the vaginal wall, uterus or top of the vagina such that there is no longer optimal support of the pelvic organs. When we treat women with pelvic organ prolapse, we are looking at ways to improve the support system of her pelvic organs and to decrease strain on the organs. The pelvic floor muscles are like a hammock or trampoline beneath the vagina, supporting the organs. Recovering optimal function, strength and responsiveness of the pelvic floor is one important component of treating the symptoms of a pelvic organ prolapse. Additionally, the hip girdles, diaphragm, abdominal muscles and low back muscles also contribute to stability and intra-abdominal pressure control. At Purple Mountain Physical Therapy we have been specialists in pelvic health for over 20 years. We have worked with many women who have POP and who are able to recover their pelvic floor and core muscle function so that they optimally support the organs and improve their ability to empty their bladder and bowels.

Constant urinary urge: If you urinate and still feel you need to go to the bathroom, pelvic health physical therapy is a good option for you. We have helped many women overcome this problem. You should be able to go to the bathroom and feel relief and no longer have a sense of urge. We will evaluate and treat you to identify what is going on and help you to get rid of this problem.
Incomplete bladder emptying: Some people experience difficulty fully emptying their bladder and may develop with recurrent urinary infections, urinary urgency or frequency and a constant sense of urinary urge. We can help identify underlying factors contributing to your incomplete bladder emptying and we will treat these and help you recover your bladder control. We recognize there may be underlying conditions, such as a neurologic condition or pelvic organ prolapse, that are contributing to your difficulty eliminating your urine and we recognize the importance of your physician providers. Even if these underlying conditions are present, there is still hope that you can improve. What we find with our patients is pelvic floor dysfunction and non-optimal urinary habits are present. We have treated many people who have successfully improved their ability to empty their bladder. Some of them have been using a catheter to urinate or to empty their bladder following urinating. These individuals are measuring the volume of urine expelled via catheter and have found objective improvements through our skilled physical therapy.

Neurogenic bladder: Individuals with neurologic conditions may experience challenges with bladder and bowel control including urinary urgency, inability to start the flow or urine and difficulty emptying their bladder. Some women may require a catheter to empty their bladder. We have worked with individuals with numerous neurologic conditions, such as following a stroke (CVA), multiple sclerosis, small fiber peripheral neuropathy and spinal cord injury. This can be a challenging condition and with the right evaluation and treatment your body may respond and you can improve your ability to urinate. As always, interdisciplinary care can provide you the best results and we are happy to communicate with your physician providers.
Nocturia: Nocturia is a condition that disrupts your sleep because you are getting up to urinate during the night. Because quality sleep is absolutely essential for our body to recover, nocturia is treatment should not be delayed, as physical therapy can help this condition. The pelvic health physical therapists at Purple Mountain physical therapy have treated many people with nocturia. Fortunately, nocturia responds very well to the skilled pelvic physical therapy we offer. In fact, some patients have reported to us that their nighttime urinating has been one of the first things to improve during the course of their physical therapy treatments! Our patients tell us the evaluation is very educational as they learn about their bladder, pelvic floor, breathing and their habits contributing to their nocturia. We recognize the importance of your other medical providers, as well, to ensure all medical causes are being addressed, also.

Persistent Genital Arousal Disorder (PGAD): We have treated women with persistent genital arousal disorder and we understand the unwanted, bothersome and distressing nature of this condition. We have advanced education in treating this condition and are members of ISSWSH, the International Society for the Study of Women’s Sexual Health and the International Pelvic Pain Society, two professional organizations that offer continuing education and advanced practice recommendations for PGAD. We have found that women with this condition have a variety of musculoskeletal impairments that benefit from pelvic health physical therapy. We utilize numerous treatments to help your persistent genital arousal disorder to calm down. Multidisciplinary care is known to be the best method of treating all pelvic pain conditions and we are happy to work with your other providers. You can expect compassionate care that is laser focused on delivering you the highest quality treatments that can deliver you results. You don’t need do suffer silently and feel alone, we are here to help you.
Chronic pelvic pain (CPP), Myofascial pain syndrome and Pelvic Pain Syndrome: If you are experiencing chronic pelvic pain or myofascial pain, we offer you expert care, focused on determining underlying contributing factors and treating these so that you can feel better. In our over 20 years of experience we have helped many women and men overcome their chronic pelvic pain and get their life back. Helping you resolve your pain and teaching you how to prevent it and moderate it, should it occur, is our goal. Typically, chronic pelvic pain and myofascial pain syndrome are multifactorial problems that may involve several systems including your pelvic floor, musculoskeletal, gynecological, urological, neurological (peripheral nerves, central nervous system and autonomic nervous system), neuroendocrine, immune and gastrointestinal. We often find patients have reduced blood flow to their myofascial tissues, underlying pelvic floor dysfunction, trigger points and myofascial restrictions in the abdomen, back, hips and thighs. The autonomic nervous system, comprised of your Sympathetic Nervous System (fight or flight) and your Parasympathetic Nervous System (Rest and Digest) can play a role in your pain. Your Vagus Nerve plays an important role in the parasympathetic nervous system and is something we can help you to improve. Through our heart rate variability coherence biofeedback training program, we can teach you to optimize your autonomic nervous system, to tonify your Vagus Nerve function, and help you to regulate and improve your body. Unraveling all that is going on can be best accomplished with interdisciplinary care and we embrace and work with your other providers to help you. Most importantly, we offer you effective treatment that can you to achieve your goals and feel better.
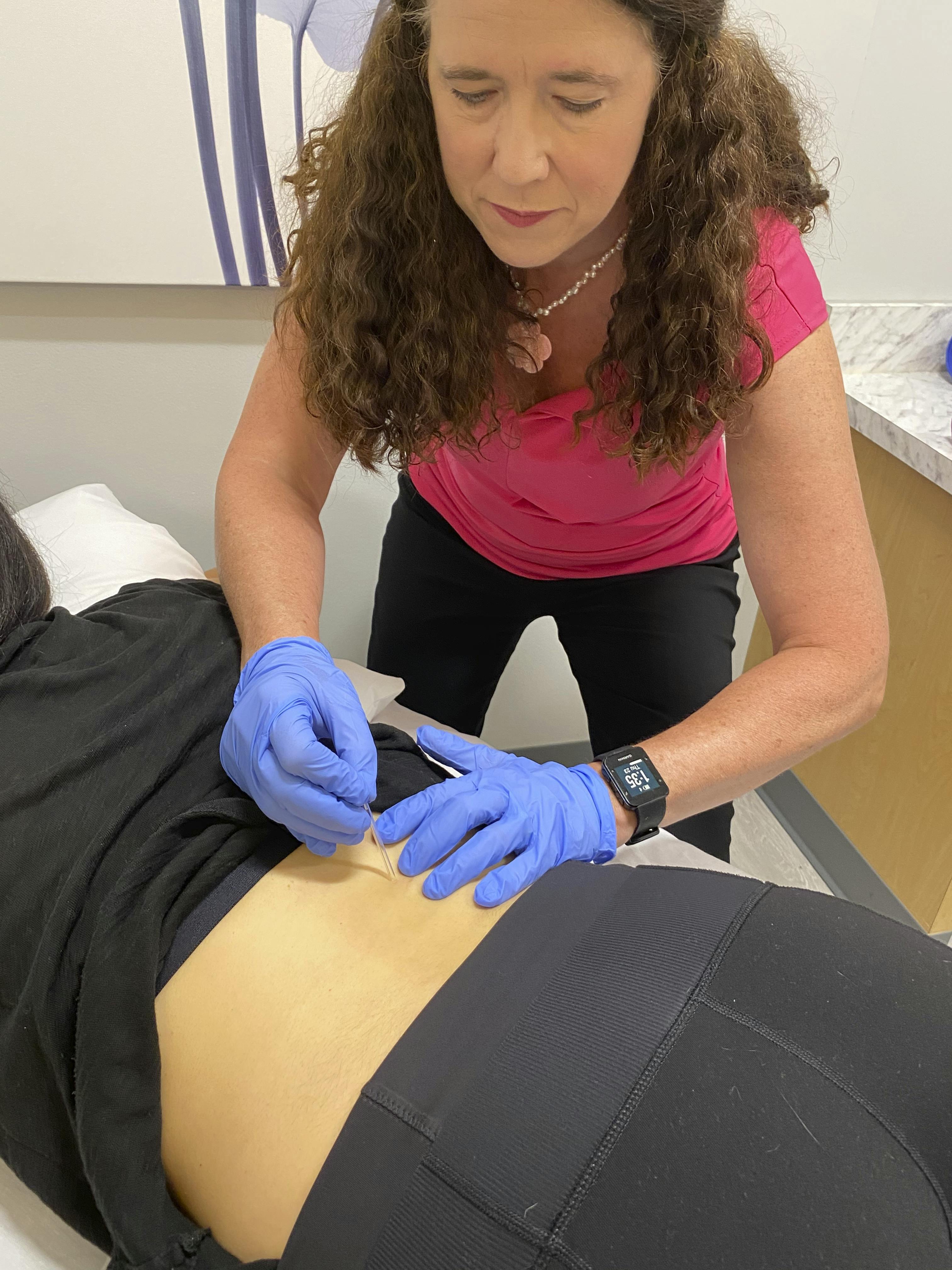
Endometriosis: Women who experience endometriosis often come to us with chronic pelvic pain, bladder or bowel challenges and sexual health concerns that they have experienced for years. Their pain might be abdominal pain that comes and goes, vaginal pain, SIJ (sacroiliac joint) pain, low back pain, hip pain or located somewhere else. The endometriosis condition has caused your musculoskeletal system to react and go into pain. It may also have set off your bladder or bowel, causing urinary or bowel symptoms, as well. This is where physical therapy can help you! We are musculoskeletal pain, bladder, bowel and pelvic health physical therapy specialists and we provide you with a proper evaluation to determine where you have myofascial restrictions, connective tissue dysfunction, trigger points, scar tissue adherence and pelvic floor dysfunction. We then treat these areas to get you relief from your pain and other symptoms. We’ve treated many women with endometriosis related chronic pain, bowel and bladder issues and have helped them restore their quality of life. We understand you might have days you want to spend in bed each month. We know you are suffering. We have heard you; we believe you and we are confident we can help you. Other women have proven this to us.
Vulvodynia, Vestibulodynia, Clitorodynia: Women who experience vulvar pain often do so silently and alone. This condition is very bothersome and there are treatments for you! Whereas vulvodynia involves pain that can be within the entire vulva (vestibule, clitoris, labia majora, labia minora) there are also what are called “localized vulvodynia” sub-categories, including vestibulodynia and clitorodynia, that are defined by one specific area that hurts you. Your pain may be provoked (meaning it hurts when it is touched) or it can be spontaneous (it hurts without any known reason) or you might have a mixture of provoked and spontaneous. Women with vulvodynia have been identified to have hypertonic pelvic floor (overactive pelvic floor) in several controlled studies. We provide experienced, expert, gentle care to evaluate you and develop a comprehensive plan of care. We find underlying factors in the myofascial tissues of the women’s abdomen, legs, hips, back and pelvic floor that perpetuate your pain. We have helped many women with this condition and we can help you, too. We value communication with your other medical providers so you can have the best outcome. There may also be underlying infectious, inflammatory or hormonal issues that are present and your physician partners are important providers for these issues.
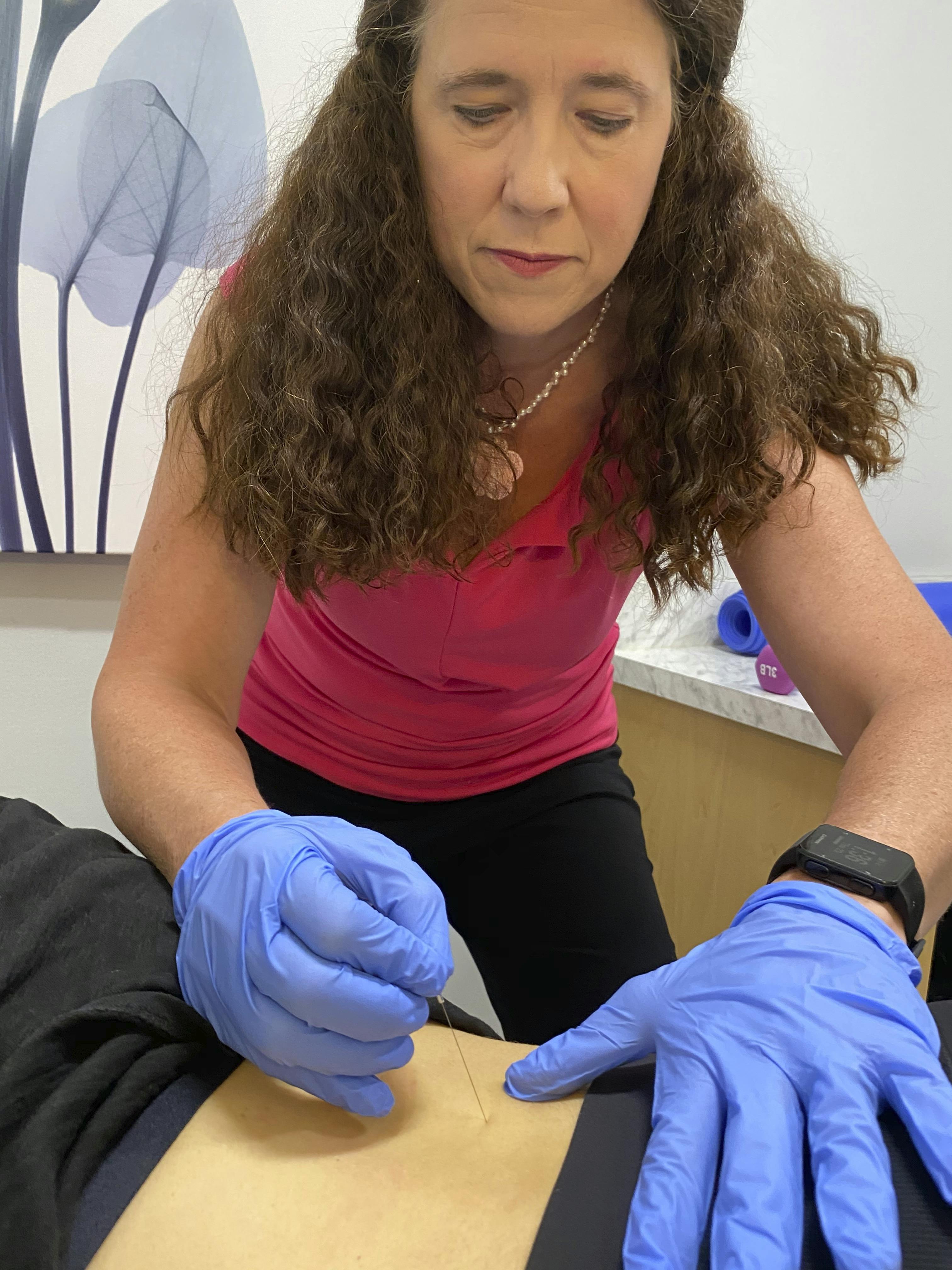
Vestibulodynia: A type of vulvodynia that exclusively involves pain in the vestibule area of the vulva, rather than the entire vulva. During your evaluation we will determine if vestibulodynia is present in your case. Your vestibulodynia might be provoked, where it hurts you if you contact it, such as inserting a tampon or attempting intercourse. Or it might be spontaneous, meaning it hurts without any known trigger. Some women have a combination of provoked and spontaneous. We will conduct a comprehensive evaluation of your pelvic floor and vulvar tissues and also your abdomen, hips, thighs and back. There is hope for your pain and we have helped many women recover from this condition.
Vaginismus: Vaginismus is a condition that causes a woman to be unable to experience vaginal penetration. Some women cannot insert a tampon due to vaginismus. Others have success with tampons, but find sexual penetration impossible or very painful and difficult. We have years of experience treating women who have vaginismus. You don’t need to suffer with this condition, there is help. Having worked with many women we understand the grief this condition generates, the loss of intimacy and the difficulty it might cause within your relationship. Women who are in their fertile years and hope to start a family are under significant stress related to this condition. We understand and we are here to help you. We will provide a gentle examination, educating you in what we find. We will evaluate your abdomen, hips, low back and thighs, as well as your pelvic area. Typically, there are myofascial and visceral restrictions in these areas contributing to your vaginismus that might include impairments in the pelvic floor, vagina and vulva, trigger points in the hips, thighs and abdomen and connective tissue restrictions in these areas. We will treat these and teach you what you can do to help yourself. We also offer specialized biofeedback for heart rate variability coherence training so you can learn to balance your autonomic nervous system and reduce your stress and anxiety related to vaginismus, so that when you are ready to attempt sexual intimacy you feel more confident in your ability to do so.
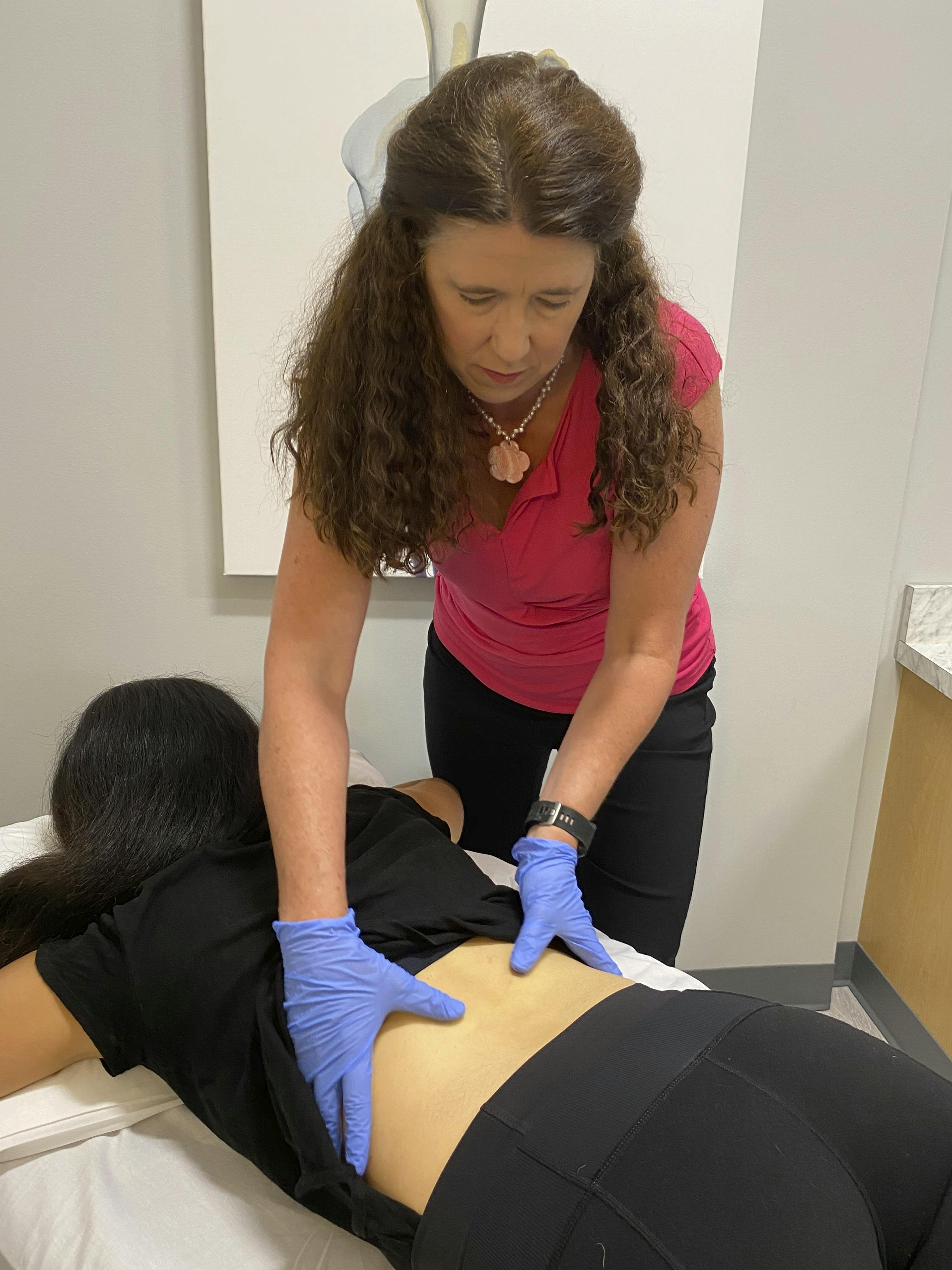
Bone health, osteopenia, osteoporosis: Bone health is an issue near and dear to our heart. We have family members who have experienced multiple, severe osteoporotic fractures and we have seen the consequences of these. Bone health is an important issue throughout a woman’s lifespan and we have concerns about young female athletes who do not experience a regular menstrual cycle because they have underlying hormonal issues and this means their estrogen levels, which are key to their developing bones, are not optimized. Women build bone until roughly 30 years of age. Lifestyle is very important for maintaining bone health. There are key things we should be doing and avoiding to optimize our bone density. As we enter midlife and menopause it becomes even more important to know how to take care of our bones. In physical therapy we can teach you key exercises that are the best for maintaining your bone health and for combatting the kyphotic, slouched, humpback that severe osteoporosis causes. If you are concerned about your bones, whether you believe them to be in good shape but simply want to keep it that way, or you have been diagnosed with osteopenia or osteoporosis, we are here to help you. We can create a custom exercise plan for you that you can take and complete as part of your fitness routine at home or the gym. We teach you how to do these exercises and we review lifestyle considerations that are key to your bone health. We are licensed physical therapists with doctoral degrees and continuing education specific to osteoporosis and we provide you a custom-made fitness program to optimize your bone health.
Urethral pain syndrome and dysuria (painful urinating): Urethral pain syndrome is quite bothersome to women, as they feel pain in the urethra and often are prescribed many courses of antibiotics that do not resolve the pain. It can be perplexing, as well, because the pain may come and go for unknown reasons. We have found that underlying pelvic floor dysfunction and pelvic myofascial restrictions, in particular high tone in the pelvic floor muscles, are typically present. This increased resting tone of the pelvic floor may also accompany increased tone of the urethral striated sphincter. When you attempt to urinate you may experience pain, even though you do not have an infection. We will evaluate you and create a treatment program to address your pelvic floor as well as myofascial tissues of your abdomen, low back, thighs and hip girdles because these areas play into your pelvic floor dysfunction. We expect your urethral pain to diminish so that you can be fit and active without fear of turning on your pain and you can urinate without wondering whether it will activate your pain.
Recurrent urinary tract infection: To be clear, if you have an infection or think you have an infection, you must see your physician and get that treated. What we treat is actually two things: First, a condition where women feel like they have an infection, but there is no infection present! Second, women who do get recurrent urinary tract infections that leave them in pain, even after the infection has resolved with medications, and they want to figure out if they have pelvic floor dysfunction or other bladder issues causing these infections. If this is you, we can help you. A woman can experience pelvic pain that mimics a urinary tract infection, even in the absence of an infection. We’ve treated many women over the years who have told us that they thought they had an infection, they did everything right by seeing their physician and getting a urine culture, but the culture came back negative. In this case typically the woman has pelvic floor dysfunction, myofascial restrictions related to the pelvis and possibly a combination of impairments in how she urinates. We can identify and treat these myofascial related issues and help you get to the bottom of your recurrent urinary tract infections. Yes, you need your physician to treat an actual infection. Yes, there can be hormone contributions to developing these infections, for which your physician and you can determine a plan. And, yes, there are often underlying musculoskeletal issues going on in your pelvis contributing to your pain and the feeling you have an infection, even when you do not. We can help you.

Hemorrhoids: If you are experiencing recurrent hemorrhoids pelvic health physical therapy may be able to help you. Hemorrhoids can be caused by improper defecation and a build up of pressure in the rectal area. If you have pelvic floor dysfunction you may have difficulty evacuating your stool effectively, causing you to strain. We can evaluate you to determine if this is the case and we can treat your pelvic floor dysfunction and teach you better strategies to defecate.
Rectocele: A rectocele occurs when your rectum bulges forward into the back wall of the vagina. What you might feel is a bulge in your vagina, especially when you have stool present. You may find it difficult to evacuate your stool, because as you attempt to defecate the stool might move more forward, towards your vagina, instead of moving outward toward the anus. Some women will place their clean fingers in their vagina and push backwards to allow the stool to expel; in effect they are relocating their rectocele to optimize the anatomic position. Pelvic health physical therapy will identify the musculoskeletal contributions to your rectocele and help you to improve these. We will also teach you optimal defecatory strategies to expel your stool without straining. We will teach you to optimize your pelvic floor, breathing and coordination of all of your core muscles. We have treated many women who have rectocele and have helped them improve their ability to defecate.
Constipation: Not only does constipation feel uncomfortable, it also can place a strain on your pelvic floor and contribute to hemorrhoids, pelvic organ prolapse and pelvic floor dysfunction. Gut health is key to overall health and if you are not experiencing regular, complete bowel movements you will have challenges to your overall wellbeing. We provide physical therapy that addresses musculoskeletal, visceral and biomechanical issues related to your constipation, including pelvic floor dysfunction. We are trained in gentle visceral mobilization and can teach you self-care techniques to help facilitate a bowel movement. We will teach you optimal strategies for expelling your stool to avoid excess strain on your pelvic floor and avoid hemorrhoids. It is important to note that for all of our patients who experience bladder conditions (urinary incontinence, urinary urgency, overactive bladder, interstitial cystitis, bladder pain, etc.) we always review and discuss gut health and constipation or diarrhea, as remedying these is important for bladder health.
IBS: Irritable bowel syndrome: Irritable bowel syndrome is a condition that often overlaps with other pelvic pain conditions. When a person has IBS, they experience recurrent episodes of abdominal pain and changes in the frequency, consistency and formation of their stool. With irritable bowel syndrome you may strain to have a bowel movement, or you might have loose stools and fecal urgency. Some people with IBS live in fear of fecal incontinence. Other people might feel cramping, abdominal pain, nausea, fatigue or fullness. The irritable bowel syndrome can “turn on” musculoskeletal pain, such that you are left with abdominal discomfort quite often, even not related to a bowel episode. We will evaluate you and determine if you have myofascial issues contributing to your symptoms. Often there is also pelvic floor dysfunction. We will discuss gut health and make recommendations for optimizing your wellbeing. As with all conditions that we treat, we are happy to partner with your other medical providers to develop a plan of care that delivers you results.
Pelvic Girdle Pain: We have helped many women overcome their pelvic girdle pain. Sometimes you hurt when you shift movements one way or another. Other times you feel an ache all the time. Your pain might be in your hips, your SI joint, your pubic bone, your pelvic floor or anywhere else in your pelvic region. We conduct a complete evaluation and develop a treatment plan, all while educating you on what we find and how you can best manage your condition so that you fully recover. We will get to the bottom of this and help you to recover so you can move, roll in bed, shift positions, climb stairs, lift items and get back to exercise without pain!
Coccydynia (coccygodynia), tailbone pain: We have treated many women with tailbone pain. Often this pain develops after labor and delivery. But you might also have it if you fall on your tailbone. Because the pelvic floor muscles are around and attach to this bone, if you have pelvic floor dysfunction it can contribute to your pain. We offer you expert care for your pain, a thorough evaluation of your coccyx, sacrum, pelvic floor dysfunction and treatment that alleviates pain. You need relief, we understand this and will provide you with a path forward. Many of our patients experience relief at each appointment and are amazed that they can sit and drive home without tailbone pain!
Dyspareunia (painful sex): If you are struggling with painful sex, we are here to help you. Often there is underlying pelvic floor dysfunction and myofascial restrictions that can be addressed to help restore your ability to engage in intimacy without clenching in pain. We will provide you with a gentle examination, education and feedback regarding our findings. Going forward, we will treat these findings and guide you in what you can do at home to help improve your condition and to take steps towards intimacy. Improving your dyspareunia will include a comprehensive treatment program to address all myofascial and visceral findings discovered in your evaluation. We understand there is fear and anxiety related to intimacy when it is painful. We also provide specialized biofeedback training in heart rate variability coherence so you can learn how to calm your fear and return to intimacy.
How do you know if you need pelvic floor PT? Click here to read this article we wrote for more information.
Purple Mountain PT is a specialty clinic located in Grand Rapids, Michigan. We help women overcome pelvic floor dysfunction, pelvic pain, bladder, bowel and intimacy related conditions. Our programs for pregnancy and postpartum recovery, bone health, treating myofascial pelvic pain, optimizing bladder control and resolving pelvic floor dysfunction have helped countless people get their lives back. If you would like to learn more you can contact us here orfeel free to fill out this online formand we will reach out to you and can connect to chat about your needs.
